Introduction. Racial and ethnic differences in risk for cardiovascular morbidity and mortality are well documented. The relative role of genetic vs environmental influences is unclear. A non-invasive measure of autonomic balance, heart rate variability (HRV) has been shown to be correlated with cardiovascular risk in some populations. Whether there are underlying differences in HRV between racial and/or ethnic groups, and whether this might therefore affect cardiovascular risk, is largely unknown.
Hypothesis. Young Asian males living in Australia for less than 5 years will have a higher HRV than long term Caucasian Australian residents.
Methods. Subjects were in two groups: 1) Caucasian males aged 18 to 25 years born in Australia (n=20); and 2) age and BMI matched Asian males resident in Australia <5 years (n=16). Subjects abstained from exercise, consuming alcohol, caffeine or guarana for 2 h prior to the experiment. After 2 min acclimatisation, either standing or supine, the subject’s ECG was recorded for 15 min and HRV analysis conducted with AD Instruments (Australia) Chart 5/HRV module. Power spectral analysis was used to derive LF:HF ratio. (LF=low frequency component; HF=high frequency component of the power spectrum.)
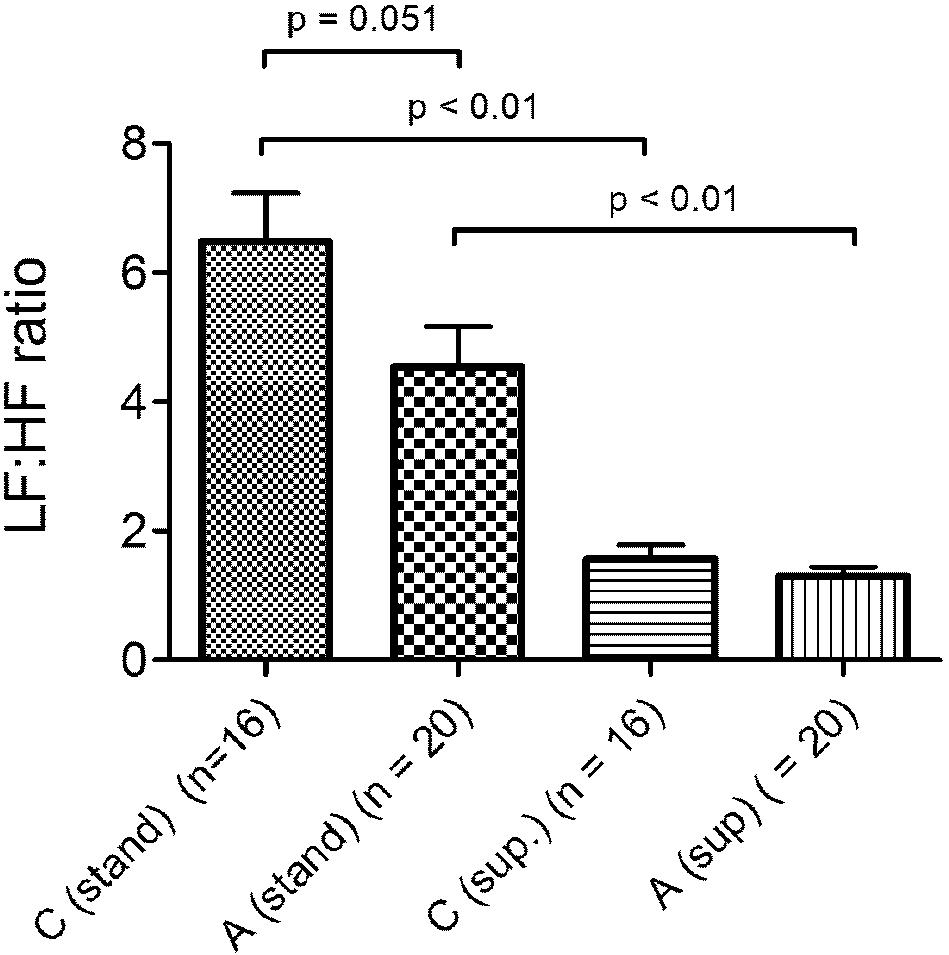
Results. There were no significant differences in age, BMI, hip:waist ratio or heart rate between the groups. For both groups there was a significant (P < 0.01) increase in LF:HF ratio when standing compared to supine. (LF:HF = 6.48 ± 0.75 standing and 1.56 ± 0.22 supine for Caucasian vs 4.54 ± 0.62 standing and 1.30 ± 0.14 supine for Asian). There was no significant difference between Caucasian and Asian groups in LF:HF ratio when supine, but when standing the data indicated that Caucasians had a higher LF:HF ratio (P = 0.051).

Conclusions. Asian subjects resident in Australia <5 years showed a reduced sympathetic drive when standing compared to Caucasian resident subjects. This may indicate a genetic difference between groups, and provide insight to the racial differences in risk for cardiovascular mortality and morbidity.